VESICULAR STOMATITIS AND COVID-19. A CASE REPORT
..................
Ana María Pérez Murcia ¹, Oscar Eduardo Mora Hernández ² , Elvis F. Gómez Osorio ³ , Laura VanessaVargas Gualdrón ³
Abstract
Keywords: Vesicular Stomatitis; Aphthous Stomatitis; Vesiculobullous Dermatoses; COVID-19; SARS-CoV-2.
..............
² Servicio de Dermatología, Hospital de San José. Decano y Especialista Dcocencia Universitaria, Fundación Universitaria de Ciencias de la Salud.
³ Servicio de Dermatología, Hospital de San José. Residente, Fundación Universitaria de Ciencias de la Salud.
ESTOMATITIS VESICULOAMPOLLOSA Y COVID-19. REPORTE DE CASO
Resumen
Introducción: La pandemia por
SARS-CoV-2 (del inglés severe acute respiratory syndrome
coronavirus 2) ha demostrado amplia variabilidad de presentaciones
clínicas multisistémicas,
siendo la piel y sus anexos uno de los órganos más afectados. Presentación del caso:Varón
de 32 años sin antecedentes conocidos, que presenta fiebre,
conjuntivitis, rinofaringoamigdalitis y lesiones orales ampollosas
extensas, que requiere hospitalización exclusiva
para manejo de las lesiones orales. Durante la hospitalización se
identifica resultado positivo
para SARS-CoV-2, sin compromiso pulmonar. Discusión: Si bien las
manifestaciones en
piel están descritas y clasificadas en la COVID-19 (del inglés
Coronavirus disease 2019), la
afectación de las mucosas, en especial en la cavidad oral son poco
frecuentes y aún no están
dilucidadas. Sin embargo, cuando ocurren generan una importante
morbilidad en el paciente,
por lo que es necesario realizar un examen físico completo para no
omitirlas y tratarlas oportunamente.
Palabras clave: Estomatitis Vesicular; Estomatitis Aftosa; Dermatopatías Vesiculoampollosas; COVID-19; SARS-CoV-2.
..................
Introduction
Since the start of the SARS-CoV-2 (severe acute respiratory
syndrome coronavirus 2) pandemic, the disease
has shown wide variability of multisystemic clinical
presentations, with the skin and its annexes being one
of the most affected organs. However, there are few reports on the
involvement of the oral mucosa, a circumstance that is likely due to
lack of inspection of this
area related to the infection risk to the examiner (1).
Numerous case reports suggest that oral mucosal changes may precede or accompany the disease without focusing on the direct impact of SARS-CoV-2 infection (2). Coinfection with other microorganisms, immunological alterations and overlapping with secondary reactions to medications have been found (3).
This article seeks to delve into the existing literature on COVID-19 (Coronavirus disease 2019) on oral mucosal lesions, in order to better understand an unusual case that required exclusive in-hospital management of oral lesions.
Clinical case
A 32-year-old male from Bogotá, Colombia with no
relevant medical history and fully vaccinated against
SARS-CoV-2 two months prior with Astrazeneca, presented to an
outpatient clinic with an eight day history
of fever, sore throat, and dry cough. The fever resolved
on day 5, but was followed by erythema and ocular
itching along with painful bullous lesions throughout
the oral mucosa prompting him to seek medical attention. The clinic
diagnosed the patient with bacterial tonsillitis and prescribed
benzathine penicillin. After
symptoms persisted for 1 more day, he sought medical
attention at the hospital.
Upon physical examination, he was afebrile, with normal respiratory rate and adequate oxygen saturation, but presented with dehydration, mild tachycardia, edema of the cheeks and inside the oral cavity (lips, cheeks, soft palate, and Stenon’s duct) exhibited tense blisters, vesicles, aphthous ulcers and unremovable yellowish-white plaques, without lingual involvement or enlarged lymph nodes (Figure 1). Signs progressed less than 24 hours following admission (Figure 2).
COVID-19 and herpetic stomatitis in probable immunosuppression were suspected, and hospitalization recommended by the Dermatology, Otorhinolaryngology and Internal Medicine services, who together initiated empirical management with analgesia, thromboprophylaxis, gastroprotection, corticosteroids, magistral formula and oral acyclovir.
Chest radiograph, Tzanck test, Human immunodeficiency virus, hepatotrophs, syphilis, viral panel, IgG and IgM (Immunoglobulin G and M) for Herpes simplex type I and II, electrolytes, liver and kidney function tests were normal.
IgG for Cytomegalovirus was positive and IgM negative. He had elevated C-reactive protein, leukocytosis (attributed to dehydration), slightly elevated glycated hemoglobin, and a positive reverse transcription-polymerase chain reaction for SARS-CoV-2.
Biopsy confirmed subepithelial bullous stomatitis with associated severe inflammatory changes, suggestive of mucosal pemphigoid, but with negative immunofluorescence. He finished management with 10 days of antiviral therapy and 15 days of corticosteroid treatment, the latter with gradual outpatient weaning, and due to improvement of lesions, he was discharged.
Discussion
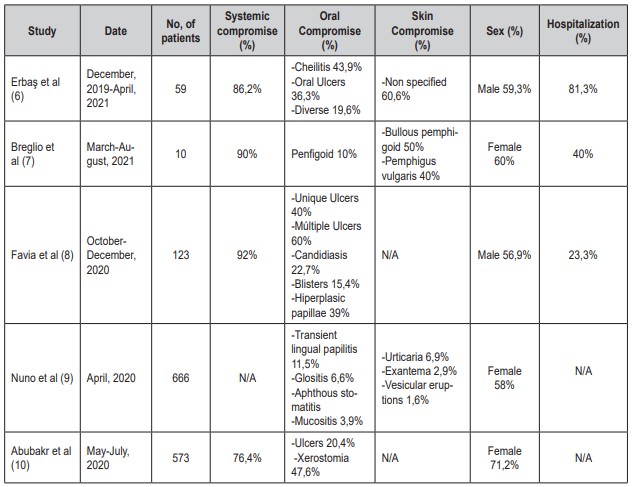
Within the spectrum of manifestations in the oral mucosa after COVID-19, the formation of blisters, aphthous ulcers, scaling gingivitis, whitish plaques, cheilitis, erythematous macules (mainly on the tongue) and enanthema have been reported in association with Kawasaki disease. These may be the only clinical manifestations of the infection or may be accompanied by other associated skin manifestations in up to 60% of the affected population (4). The most frequent locations within the oral cavity are the palate and tongue, followed by the gums and lips, with a resolution time of 3 to 21 days spontaneously or with pharmacological treatment (5). Oral manifestations are described in Table 1 (6-10).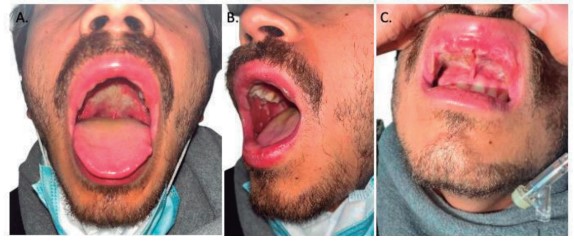
Figure 1. Upon hospital admission (Fourth day of oral lesions). Tense blisters with serous content are evident on the upper lips, and well-defined whitish plaques with irregular edges on the soft palate (A). Presence of tense blisters with serous content on the upper lips, and scarce on bilateral cheeks, well defined but unremovable whitish plaques (B). Vesicles, tense blisters with serous content, and large well-defined whitish plaques with irregular edges are evident on the mucosa (C)
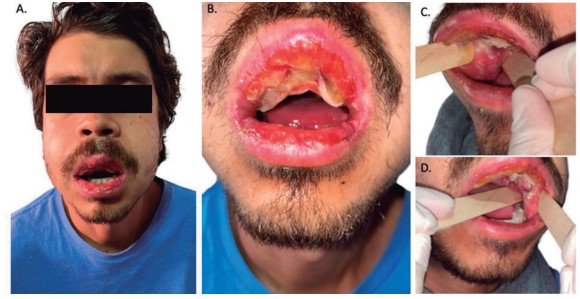
Figure 2. Twelve hours of hospital admission (Fifth day of oral lesions). Increased edema in the lower two thirds of the face (A). In the upper lips, abundant yellow and whitish membranes are evident, associated with multiple erosions also present in the lower lips (B). In bilateral cheeks and on Stenon’s duct, abundant whitish plaques with irregular and well-defined borders (C, D).
Although the pathophysiology of blister formation in the oral cavity after COVID-19 infection has not been fully elucidated, it can be explained by the angiotensin converting enzyme II and the serine transmembrane protease 2, required for the cellular entry of SARSCoV-2, which are found diffusely in the oral mucosa and are related to a hyperinflammatory state that ends in the deregulation of oral keratinocytes (11). Coagulation disorders associated with COVID-19 can also trigger the development of necrotic ulcers in the oral mucosa, due to the reactivation of infectious entities such as herpes, and mycosis, after immunological deterioration and dysbiosis secondary to the management of COVID-19 (6).
Bullous pemphigoid is a rare autoimmune disorder directed against hemidesmosomes of the skin with the appearance of tense blisters, that in up to 15% of cases, may present oral manifestations. This disorder can be triggered by COVID-19 (3) in relation to a cross-reactivity of antibodies or activated lymphocytes with antigens containing similar epitopes (12), giving a higher mortality rate (8). It is more common to observe reports of its development after the application of the SARS-CoV-2 vaccine (13), although it has been reported mainly in patients with previous subclinical or eczematous manifestations (14).
There is no treatment for the patient with oral manifestations due to COVID-19, and insufficient studies in relation to therapeutic management. Resolution of the triggering and/or underlying factors are key to the reduction of these lesions, among them: optimization of the oral hygiene, identification and treatment of opportunistic infections, stress reduction, stabilization of underlying diseases, avoid trauma, and reduce vascular compromise as well as the hyperinflammatory response (systemic corticosteroids) (15).
Table 1. Oral mucosal and skin changes in COVID-19.
In the case of the patient in question, he presented conjunctivitis, fever, oral lesions and upper respiratory tract symptoms associated with COVID-19, but there was no involvement of the lung parenchyma. It was also not possible to identify a viral or autoimmune etiology that would explain the result of the pathology suggestive of mucosal pemphigoid, which cannot rule out these entities or confirm that it is caused by SARSCoV-2. What is evident is the relationship between the appearance of oral lesions and COVID-19 due to the timing of their appearance generated either by secondary immunosuppression that promotes co-infection, by triggering autoimmunity and/or by intrinsic damage of the virus.
In conclusion, there are many systemic manifestations currently related to SARS-CoV-2 infection. Although the manifestations on the skin have been described and classified, the involvement of the mucous membranes, especially the oral cavity, are rare and have not yet been elucidated. However, when they occur, they generate significant morbidity in the patient, preventing oral feeding and administration of oral treatment, therefore necessary to perform a complete physical examination to avoid omitting them and thus be able to give adequate and timely management.
Patient Consent
Written informed consent was obtained from the patient for publication of this case report and accompanying images. A copy of the written consent is available for review by the editor-in-chief of this journal upon request
Referencias
1.Carreras-Presas CM, Sánchez JA, López-Sánchez AF,
Jané-Salas E, Somacarrera Pérez ML. Oral vesiculobullous lesions
associated with SARS-CoV-2 infection.
Oral Dis. 2021;27(Suppl 3):710-2.
2. Ortiz L, Morales L, Palazuelos R. Papel de los tejidos orales durante la infección por SARS-CoV-2. Rev. ADM. 2021;: 167-75.
3. Olson N, Eckhardt D, Delano A. New-Onset Bullous Pemphigoid in a COVID-19 Patient. Case Rep Dermatol Med. 2021;2021:5575111.
4. Subramaniam T, Nikalje 1 MR, Jadhav 2 S. Oral manifestations among COVID 19: An observational study of 713 patients. Dental Research Journal; 2021;:1-7.
5. Paradowska-Stolarz AM. Oral manifestations of COVID-19: Brief review. Dent Med Probl. 2021;58(1):123-6.
6. Erbaş GS, Botsali A, Erden N, Arı C, Taşkın B, Alper S, et al. COVID-19-related oral mucosa lesions among confirmed SARS-CoV-2 patients: a systematic review. Int J Dermatol. 2022;61(1):20-32.
7. Breglio KF, Sarver MM, Hall RP, Marano AL. SARSCoV-2 infections in patients with autoimmune blistering disorders: a case series and retrospective analysis. JAAD Int. 2022;7:38-43.
8. Favia G, Tempesta A, Barile G, Brienza N, Capodiferro S, Vestito MC, et al. Covid-19 Symptomatic Patients with Oral Lesions: Clinical and Histopathological Study on 123 Cases of the University Hospital Policlinic of Bari with a Purpose of a New Classification. J Clin Med. 2021;10(4):757.
9. Nuno A, Martín P, Magaletsky K, Martín M, Herránz C, Artigas J, et al. Prevalencia de manifestaciones mucocutáneas en 666 pacientes con COVID-19 en un hospital de campaña en España: hallazgo oral y palmoplantares. Br J Dermatol. 2021;184(19:184-5.
10. Abubakr N, SalemZA, Kamel AHM. Manifestaciones orales en casos leves a moderados de infecci n viral por COVID-19 en la población adulta. Dent Med Probl. (2021)58(1):7–15.
11. Orilisi G, Mascitti M, Togni L, Monterubbianesi R, Tosco V, Vitiello F, et al. Oral Manifestations of COVID-19 in Hospitalized Patients: A Systematic Review. Int J Environ Res Public Health. 2021;18(23).
12. Rosińska-Więckowicz A, Jałowska M, Bowszyc-Dmochowska M, Dmochowski M. Case Report: Infantile Bullous Pemphigoid: Triggering by COVID-19 Is Speculative. Front Med. 2021;8:760823.
13. Pérez-López I, Moyano-Bueno D, Ruiz-Villaverde R. [Bullous pemphigoid and COVID-19 vaccine]. Med Clin (Barc). 2021;157(10):e333-e4.
14. Damiani G, Pacifico A, Pelloni F, Iorizzo M. The first dose of COVID-19 vaccine may trigger pemphigus and bullous pemphigoid flares: is the second dose therefore contraindicated? J Eur Acad Dermatol Venereol. 2021;35(10):e645-e7.
15. Cuevas-Gonzalez MV, Espinosa-Cristóbal LF, DonohueCornejo A, Tovar-Carrillo KL, Saucedo-Acuña RA, García-Calderón AG, et al. COVID-19 and its manifestations in the oral cavity: A systematic review. Medicine (Baltimore). 2021;100(51):e28327.
Recibido: 28 de
febrero de 2022
Aceptado: 15 de marzo de 2022
Correspondencia:
Ana María Pérez Murcia
amperez1@fucsalud.edu.co
Aceptado: 15 de marzo de 2022
Correspondencia:
Ana María Pérez Murcia
amperez1@fucsalud.edu.co